Bottom line
To date we are seeing a small reduction in Covid-19 prevalence in England, the number of asymptomatic patients being about 13% of those who test positive for SARS-CoV-2. Applying a prediction interval to the latest systematic review suggests the chance of encountering an asymptomatic patient varies between 1% and 78% of those who would test positive. Without rapid and accurate virus and antibody testing at present extreme care still needs to be taken regarding dental aerosol generating procedures to protect both patients and staff. Self-reporting infection without a confirmatory test is about 3% accurate.
Introduction
As with all Covid-19 related data more information is appearing and being updated every day. In this opinion paper I would like to discuss the differences between Covid-19 positive patients who are asymptomatic/presympromatic, and symptomatic; what the latest data locally and globally shows, and how to interpret the data presented when making clinical decisions of individual patient risk.
Methods
The definition of a presymptomatic patient is a person where SARS-CoV-2 is detected before symptom onset, and asymptomatic are persons where SARS-CoV-2 is detected but symptoms never develop. Symptomatic is therefore those persons where SARS-CoV-2 is detected, and they have symptoms (Furukawa et al., 2020). In a cross-sectional study, one cannot separate the two categories of asymptomatic and presymptomatic as the data collected only refers to a specific time point such as the 3rd of May. If a longitudinal study is undertaken over a couple of weeks, then it may be possible to detect the patients who later go on to develop symptoms.
The latest data from the ONS, updated on the 28th May revised its prevalence estimate down to 0.24% of the community with COVID-19 (95% confidence interval: 0.11% to 0.46%) based on tests performed on 18,913 people in 8,799 households (ONS, 2020). Between the 26th April and the 25th May of those participants who reported symptoms 2.62% (95% CI: 1.56% to 4.11%) also tested positive, compared to an estimate of 0.35% of those not reporting any symptoms on the day of the test (95% CI: 0.30% to 0.47%). From this we could conclude that the sensitivity of self-reporting coronavirus infection without a confirmatory test is 2.62% accurate, and of those individuals with a positive test 13.36% were asymptomatics on the day (both true asymptomatics and presymptomatics).
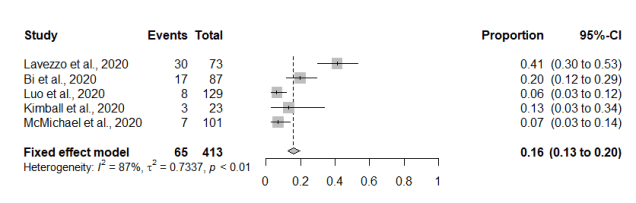
A recent systematic review by Byambasuren and co-workers set out to estimate the extent of true asymptomatic individuals and the associated risk of community spread (Byambasuren et al., 2020). Their inclusion criteria required people of any age who were at-risk of contracting SARS-CoV-2 virus, and diagnosed by laboratory-based real time quantitative reverse transcription polymerase chain reaction (RT-qPCR) or serological tests to be positive. These people remained symptomless throughout the follow up period of at least 7 days to distinguish them from pre-symptomatic cases. From the 5 papers that fulfilled these criteria they undertook a meta-analysis and concluded using a fixed-effect model that the proportion of asymptomatic cases was 16% (95% CI: 12% – 20%) (See Figure 1.)
Figure 1.Fixed effects pooled estimates of proportion of asymptomatic carriers
The authors used a fixed effects model possibly due to the small number of studies with similar methodologies. If, however a prediction interval (Borenstein et al., 2011) was added to the same data using the ‘meta’ package in R the summary estimate remains the same but the distribution of true effect sizes one could expect in future studies could be as low as 1% and as high as 78% (See Figure 2.).
Figure 2. Fixed effects pooled estimates of proportion of asymptomatic carriers plus prediction interval

Discussion
When interpreting the summary estimate within a systematic review it must be remembered this represents the mean and error variability between the different study results, and not the true distribution of asymptomatic Covid-19 carries that one may encounter tomorrow in your practice. In other words, it would not be impossible for you to encounter a group of patients (say a family) where 78% are true asymptomatic patients. As researchers produce more high-quality studies (preferably ≥24) this prediction interval will drop sharply down but unlike a confidence interval never approach zero.
References
BORENSTEIN, M., HEDGES, L. V., HIGGINS, J. P. & ROTHSTEIN, H. R. 2011. Prediction IntervalsI. Introduction to meta-analysis. John Wiley & Sons.
BYAMBASUREN, O., CARDONA, M., BELL, K., CLARK, J., MCLAWS, M.-L. & GLASZIOU, P. 2020. Estimating the extent of true asymptomatic COVID-19 and its potential for community transmission: systematic review and meta-analysis. medRxiv.
FURUKAWA, N., BROOKS, J. & SOBEL, J. 2020. Evidence Supporting Transmission of Severe Acute Respiratory Syndrome Coronavirus 2 While Presymptomatic or Asymptomatic. Emerging infectious diseases, 26.
ONS. 2020. Coronavirus (COVID-19) Infection Surveypilot: England, 28 May 2020 [Online]. Available: https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/conditionsanddiseases/bulletins/coronaviruscovid19infectionsurveypilot/28may2020 [Accessed].
Disclaimer: The article has not been peer-reviewed; it should not replace individual clinical judgement, and the sources cited should be checked. The views expressed in this commentary represent the views of the author and not necessarily those of the host institution. The views are not a substitute for professional advice.